- Tissue engineering (TE) is an interdisciplinary field that applies the principles of engineering and the life sciences toward the development of biological substitutes.
- Stem cells: undifferentiated or partially differentiated cells that can differentiate into various types of cells and proliferate indefinitely to produce more of the same stem cell.
- Induced Pluripotent stem cells (iPS) can then be directed to differentiate into the three main cell types found in the central nervous system (neurons, oligodendrocytes, and astrocytes)
- Due to the poor treatment outcomes of in situ neural stem cell regeneration, nerve injuries and neurodegenerative illnesses remain as severe concerns.
- Several studies have examined the use of embryonic stem cells for neural tissue engineering applications with a focus on diseases and disorders that affect the central nervous system.
- Recent development of induced pluripotent stem cells along with tissue engineered scaffolds provides an intriguing alternative to the use of human embryonic stem cell lines for these applications!
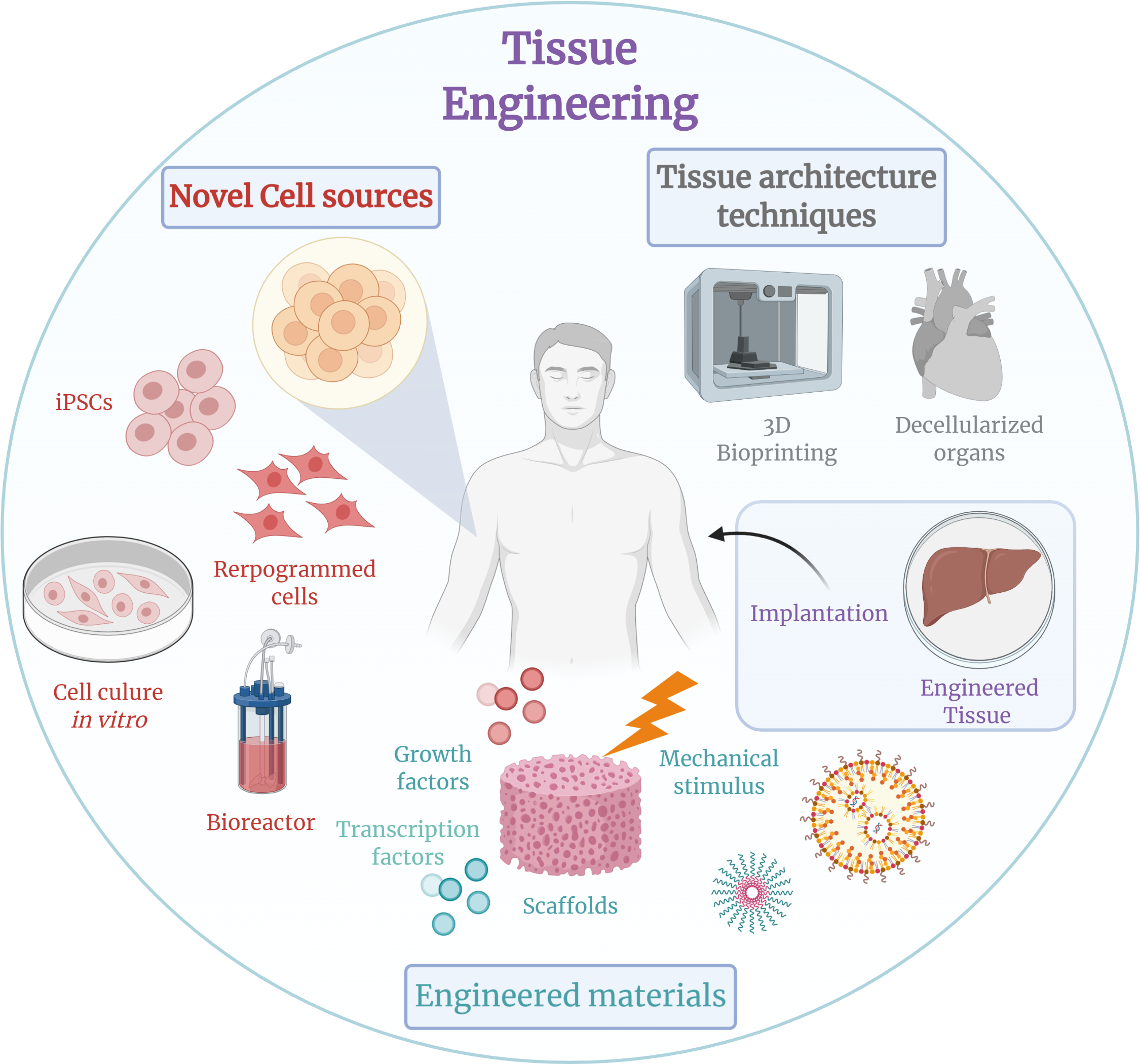
Tissue Engineering
Tissue engineering is a biomedical engineering discipline that restores, maintains, improves, or replaces biological tissues using a combination of cells, engineering, materials, technologies, and appropriate bio-chemical and physicochemical parameters. Tissue engineering is most commonly associated with the use of cells on tissue scaffolds in the formation of new viable tissue for medical purposes, but it is not limited to celland tissue scaffold applications.
3D bioprinting is a cutting-edge biomanufacturing platform that allows living cells, signalling molecules, and biomaterials to be deposited using computer-aided design (CAD) to create tissue engineered constructs with precise tissue architecture (Murphy and Atala 2014, Ashammakhi, Hasan et al. 2019). Bioprinting technology can create graded macroscale architectures that mimic the ECM, allowing different cell types to attach and proliferate at the same time (Augustine, Kalva et al. 2021). Furthermore, bioprinted models must have spatial control of matrix properties, the ability to integrate perfusable vascular networks, automation, and high-throughput testing capabilities for determining metabolic and toxicological properties (Datta, Dey et al. 2020).
SCAFFOLDS
Scaffolds are materials that have been engineered to contribute to the formation of new functional tissues for medical purposes by causing desirable cellular interactions. Cells are frequently ‘seeded’ into these structures capable of supporting the formation of three-dimensional tissue. Scaffolds mimic the native tissue’s extracellular matrix, simulating the in vivo environment and allowing cells to control their own microenvironments.
Scaffolds must meet certain requirements in order to achieve the goal of tissue reconstruction. To facilitate cell seeding and diffusion throughout the entire structure of both cells and nutrients, high porosity and adequate pore size are required. Biodegradability is frequently an important consideration, as scaffolds should ideally be absorbed by the surrounding tissues without the need for surgical intervention. The rate of degradation must be as close to that of tissue formation as possible: this means that while cells are constructing their own natural matrix structure around themselves, the scaffold can provide structural integrity within the body and will eventually break down, leaving newly formed tissue to take over the mechanical load.
Injectability is also critical for clinical applications. Recent research on organ printing has demonstrated how critical it is to maintain good control of the 3D environment in order to ensure experiment reproducibility and provide better results.
Neural Tissue Engineering
With the start of the first clinical trial evaluating a human embryonic stem (ES) cell-derived therapy for the treatment of acute spinal cord injury (SCI), a number of studies have looked into how to direct embryonic cells to differentiate into specific neural phenotypes using a variety of cues in order to replace diseased or damaged neural tissue. Furthermore, the recent development of induced pluripotent stem cells offers an intriguing alternative to using human embryonic stem cell lines for these purposes.
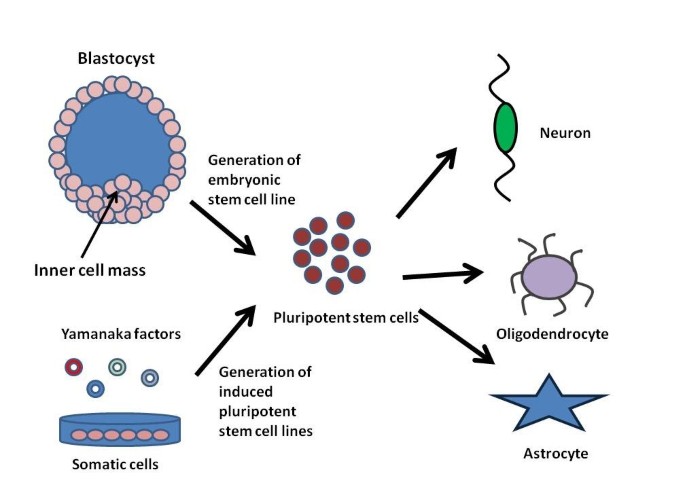
For the treatment of SCI, several groups have used tissue engineering approaches that combine biomaterial scaffolds with ES cells. The Sakiyama-Elbert group used a fibrin-based scaffold to deliver growth factors that promote the differentiation of ES cells into neurons and oligodendrocytes, and this approach was shown to improve functional recovery in a rat model of SCI.
The Baharvand group investigated the transplantation of neural progenitors derived from human ES cells inside collagen scaffolds for the treatment of SCI, and found that this approach improved locomotor function after transplantation.
In an in vitro setting, another group created electrospun poly ()-caprolactone scaffolds that supported mouse ES cell culture and promoted differentiation into nestin-positive neural progenitors. Unlike traditional ES cell lines, iPS cells allow for the generation of pluripotent cell lines without the use of embryos, as well as the creation of patient-specific iPS cell lines, which should reduce the risk of transplant rejection.
iPS cells and their ability to differentiate into neural phenotypes have been studied in a number of studies. A recent study found that human iPS cells use the same transcription networks as traditional human ES cell lines for neural differentiation. In work done by Yamanaka, 36 mouse iPS cell lines were evaluated to determine their potential for generating neural phenotypes after secondary neurosphere formation, as well as their potential safety for transplantation as indicated by teratoma formation in an in vivo setting. These cell lines showed the ability to differentiate into the three cell types found in the CNS (neurons, oligodendrocytes, and astrocytes) after a retinoic acid induction period, and certain iPS cell lines did not form teratomas after implantation, making them a ‘safe’ cell line.
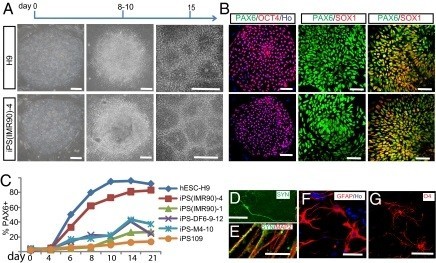
Overall, there is a large body of evidence demonstrating the feasibility of using pluripotent stem cells to produce CNS replacement tissue. The current evaluation of oligodendrocytes derived from human ES cells shows that this technology holds promise for the treatment of SCI and other neurological disorders and diseases, while the development of iPS cell lines now allows for the production of patient-specific neural tissue derived from pluripotent stem cells.
Supplementary material
REFERENCES
Cheng, Hong, et al. “Electrical Stimulation Promotes Stem Cell Neural Differentiation in Tissue Engineering.” Stem Cells International, vol. 2021, 20 Apr. 2021, pp. 1–14, downloads.hindawi.com/journals/sci/2021/6697574.pdf, 10.1155/2021/6697574. Accessed 28 June 2021.
Newman, Peter, et al. “Carbon Nanotubes: Their Potential and Pitfalls for Bone Tissue Regeneration and Engineering.” Nanomedicine: Nanotechnology, Biology and Medicine, vol. 9, no. 8, Nov. 2013, pp. 1139–1158, http://www.sciencedirect.com/science/article/pii/S1549963413002694?via%3Dihub, 10.1016/j.nano.2013.06.001. Accessed 28 June 2021.
Willerth, Stephanie M. “Neural Tissue Engineering Using Embryonic and Induced Pluripotent Stem Cells.” Stem Cell Research & Therapy, vol. 2, no. 2, 2011, p. 17, stemcellres.biomedcentral.com/articles/10.1186/scrt58, 10.1186/scrt58. Accessed 28 June 2021.
—. “Neural Tissue Engineering Using Embryonic and Induced Pluripotent Stem Cells.” Stem Cell Research & Therapy, vol. 2, no. 2, 2011, p. 17, stemcellres.biomedcentral.com/articles/10.1186/scrt58, 10.1186/scrt58. Accessed 1 July 2021.
Johnson PJ, Parker SR, Sakiyama-Elbert SE: Fibrin-based tissue engineering scaffolds enhance neural fiber sprouting and delay the accumulation of reactive astrocytes at the lesion in a subacute model of spinal cord injury. J Biomed Mater Res A. 2010, 92: 152-163.
Johnson PJ, Tatara A, McCreedy DA, Shiu A, Sakiyama-Elbert SE: Tissue-engineered fibrin scaffolds containing neural progenitors enhance functional recovery in a subacute model of SCI. Soft Matter. 2010, 6: 5127-5137. 10.1039/c0sm00173b.
Johnson PJ, Tatara A, Shiu A, Sakiyama-Elbert SE: Controlled release of neurotrophin-3 and platelet-derived growth factor from fibrin scaffolds containing neural progenitor cells enhances survival and differentiation into neurons in a subacute model of SCI. Cell Transplant. 2010, 19: 89-101. 10.3727/096368909X477273.
Willerth SM, Arendas KJ, Gottlieb DI, Sakiyama-Elbert SE: Optimization of fibrin scaffolds for differentiation of murine embryonic stem cells into neural lineage cells. Biomaterials. 2006, 27: 5990-6003. 10.1016/j.biomaterials.2006.07.036.
Hatami M, Mehrjardi NZ, Kiani S, Hemmesi K, Azizi H, Shahverdi A, Baharvand H: Human embryonic stem cell-derived neural precursor transplants in collagen scaffolds promote recovery in injured rat spinal cord. Cytotherapy. 2009, 11: 618-630. 10.1080/14653240903005802.
Hu BY, Weick JP, Yu J, Ma LX, Zhang XQ, Thomson JA, Zhang SC: Neural differentiation of human induced pluripotent stem cells follows developmental principles but with variable potency. Proc Natl Acad Sci USA. 2010, 107: 4335-4340. 10.1073/pnas.0910012107.
Murphy, S. V. and A. Atala (2014). “3D bioprinting of tissues and organs.” Nat Biotechnol 32(8): 773-785.
Ashammakhi, N., A. Hasan, O. Kaarela, B. Byambaa, A. Sheikhi, A. K. Gaharwar and A. Khademhosseini (2019). “Advancing Frontiers in Bone Bioprinting.” Advanced Healthcare Materials 8(7): 1801048.
Augustine, R., S. N. Kalva, R. Ahmad, A. A. Zahid, S. Hasan, A. Nayeem, L. McClements and A. Hasan (2021). “3D Bioprinted cancer models: Revolutionizing personalized cancer therapy.” Translational Oncology 14(4): 101015.
Datta, P., M. Dey, Z. Ataie, D. Unutmaz and I. T. Ozbolat (2020). “3D bioprinting for reconstituting the cancer microenvironment.” npj Precision Oncology 4(1): 18.
Featured Image Credit HQuality / Shutterstock
More From The NeuroBlog
- How can Neurofilament light concentrations help in Diagnosis?Overview In May 2022, I attended a conference in Syndey, Australia. The conference was targeted mainly for psychiatrists and neuropsychiatrists. I was able to attend this lovely conference through my company called Monarch Mental Health Group. On the first day, the conference kicked off by an invited keynote speaker. This speaker was a psychiatrist, and … Continue reading How can Neurofilament light concentrations help in Diagnosis?
- Execessive Neural Noise in Developmental Dyslexia?Overview Developmental dyslexia (reading disabilities/disorders, or decoding-based reading disorder) is a neurodevelopmental disorder with multiple potential underlying genetic, neural, and cognitive factors. Past models have not been very successful at integrating key neural and behavioural features of dyslexia with common neural processes, until Hancock et al. (2017) proposed their dyslexia model. Dyslexia risk genes indicate … Continue reading Execessive Neural Noise in Developmental Dyslexia?
- Debunking Popular Neuromyths: Do You Use Your Entire Brain?It is the summer of 2014 on Earth’s Northern hemisphere and the movie Lucy is hitting theatres. The official promotional posters and movie trailers contain the tagline “The average person uses 10% of their brain capacity. Imagine what she could do with 100%.” Lucy becomes the second most successful debut for a French action film, … Continue reading Debunking Popular Neuromyths: Do You Use Your Entire Brain?
